• Introduction
• Understanding Your Heart Condition
• Post-Diagnosis Emotional Support
• Lifestyle Changes for Heart Health
• How a Visit to a Cardiologist Would Help You or Ease Anxiety
• Medication Adherence and Monitoring
• Building a Support Network
• Practical Tips for Daily Living
• Monitoring Your Symptoms and Knowing When to Seek Help
• Planning for the Future
• Conclusion
Introduction
Being diagnosed with a heart condition can be a life-changing experience and often brings with it a range of emotions and uncertainties. It is important to recognize that this is a significant event that demands proper attention and care.
Individuals living with a heart condition require effective post-diagnosis support and management. The proper guidance and implementation of necessary lifestyle changes can significantly enhance overall well-being and quality of life.
Understanding Your Heart Condition
What Exactly is a Heart Condition?
A heart condition refers to a wide range of disorders affecting the heart’s function and structure. These conditions can affect the heart’s electrical system or the blood vessels responsible for supplying it with oxygen and nutrients.
Types of Heart Conditions and Their Implications
Common heart conditions include coronary heart disease, heart failure, arrhythmias (irregular heartbeats), and congenital heart defects. Each condition has its unique characteristics, symptoms, and potential implications for overall health and well-being.
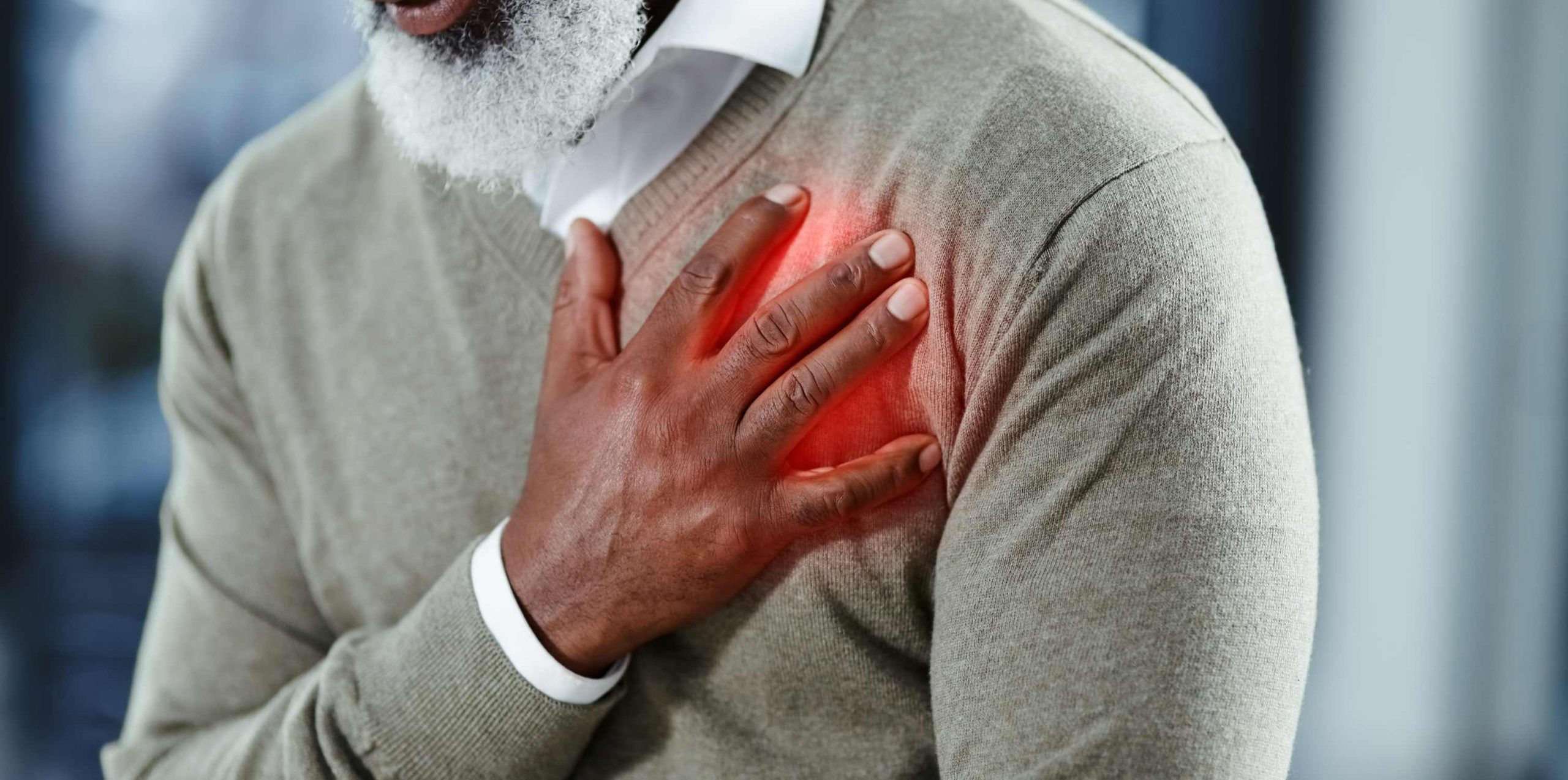
Common Symptoms and Warning Signs
It is essential to be aware of the common symptoms and warning signs associated with heart conditions, such as chest pain, shortness of breath, irregular heartbeats, fatigue, and swelling in the legs or ankles. Recognizing these signs early can aid in prompt heart disease diagnosis and treatment.
Post-Diagnosis Emotional Support
The Emotional Impact of a Heart Condition
Receiving a diagnosis for a heart condition can be an overwhelming experience. It is natural to feel a range of emotions, such as anxiety, fear, sadness, and even denial. However, it is important to acknowledge and address these feelings appropriately.
Coping Strategies for Dealing with Emotional Stress
Various coping strategies can help individuals manage the emotional stress associated with a heart condition diagnosis. These may include practicing mindfulness and relaxation techniques, seeking support from loved ones, and engaging in enjoyable activities that promote a positive mindset.
The Importance of Seeking Professional Help
If emotional challenges become overwhelming, it is crucial to seek professional help from a therapist or counselor. They can provide valuable guidance and support in navigating the emotional journey and developing effective coping mechanisms.
Lifestyle Changes for Heart Health
Dietary Modifications for a Healthy Heart
Adopting a heart-healthy diet is essential for managing and potentially improving heart condition. This may involve reducing the intake of saturated fats, sodium, and added sugars while increasing the consumption of fruits, vegetables, whole grains, and lean proteins.
Importance of Regular Exercise and Physical Activity
Regular physical activity and exercise can greatly benefit individuals with heart conditions. It can improve cardiovascular health, strengthen the heart muscle, and reduce risk factors associated with heart disease. However, it is crucial to consult with a healthcare provider to develop an appropriate exercise plan tailored to individual needs and limitations.
Managing Stress and Its Effect on Heart Health
Chronic stress can negatively impact heart health by elevating blood pressure, increasing inflammation, and contributing to unhealthy behaviors. Learning effective stress management techniques, such as deep breathing exercises, meditation, or yoga, can help mitigate the adverse effects of stress on the heart.
The Role of Sleep in Heart Condition Management
Lack of sleep can contribute to various cardiovascular risk factors, such as high blood pressure, inflammation, and obesity. Prioritizing good sleep hygiene and addressing any sleep-related disorders can support heart condition management.
How a Visit to a Cardiologist Would Help You or Ease Anxiety
Seeking the expertise of a cardiologist can be instrumental in managing a heart condition and alleviating anxiety or concerns related to your diagnosis. Here are some ways a visit to a cardiologist can help:
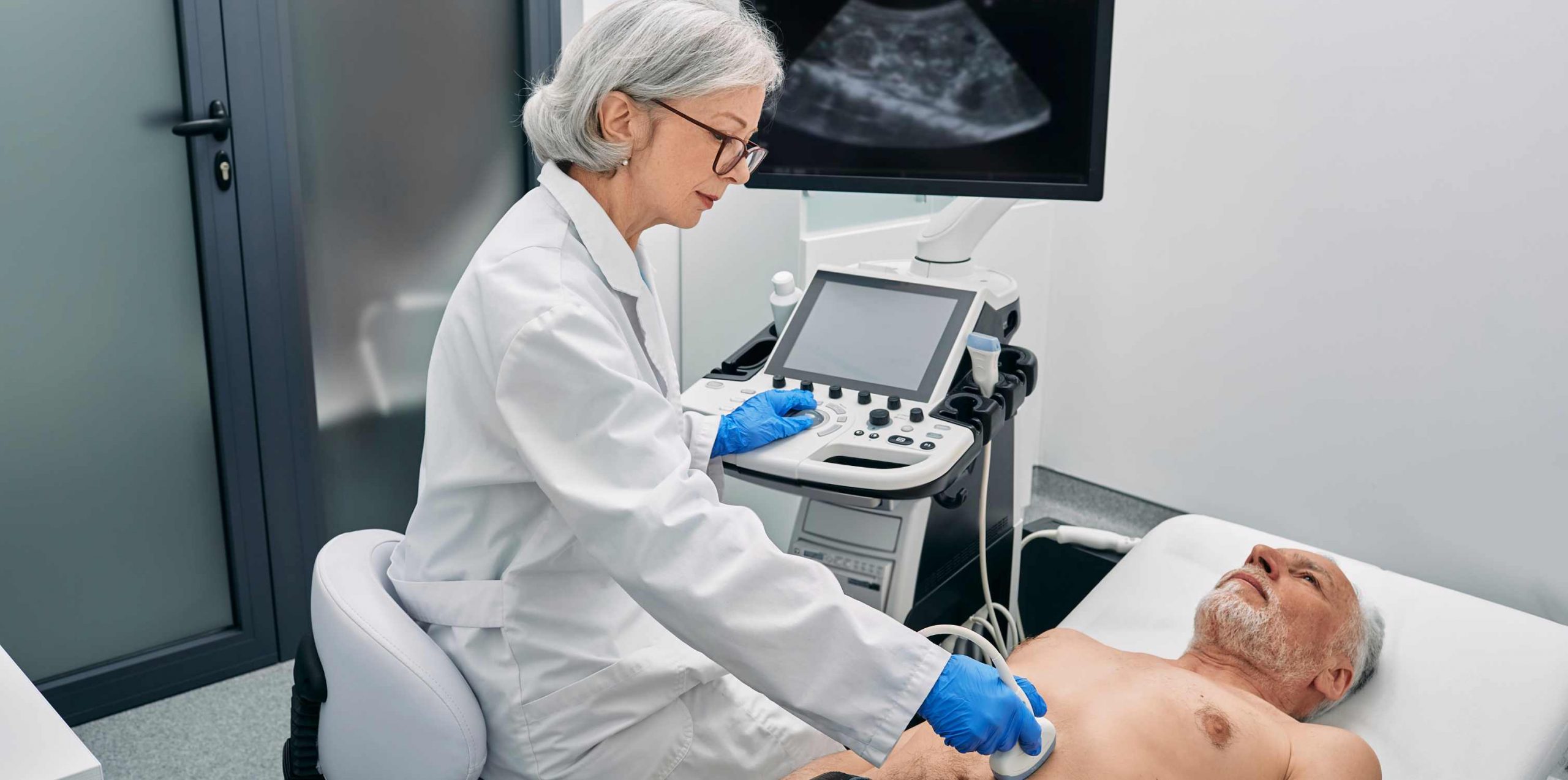
1. Comprehensive Evaluation:
A cardiologist can perform a thorough evaluation, including physical examinations, diagnostic tests, and a review of your medical history. This comprehensive assessment helps identify the specific type and severity of your heart condition, providing clarity and enabling the development of an individualized treatment plan.
2. Expert Guidance and Personalized Treatment:
Cardiologists are specialists in the diagnosis, treatment, and management of heart conditions. They can provide expert guidance on the most appropriate medical interventions, such as medications, lifestyle modifications, or surgical procedures, tailored to your specific needs and circumstances.
3. Explanation of Your Condition:
A cardiologist can clearly explain your heart condition, its causes, symptoms, and potential implications. Understanding your condition better can help alleviate anxiety and empower you to take an active role in your care.
Addressing Concerns and Answering Questions: During your visit, you will have the opportunity to ask questions and address any concerns you may have about your diagnosis, treatment options, or long-term prognosis. Receiving accurate and comprehensive information from a medical expert can provide reassurance and clarity.
4. Ongoing Monitoring and Follow-up Care:
Cardiologists can closely monitor your condition over time, making adjustments to your treatment plan as needed. Regular follow-up visits allow for the early detection of any changes or complications, enabling timely interventions and ensuring optimal management of your heart health.
5. Emotional Support and Counseling:
In addition to medical expertise, many cardiologists and their healthcare teams provide emotional support and counseling to help patients cope with the psychological impacts of living with a heart condition. They can offer strategies for managing stress, anxiety, and depression, which are common challenges faced by individuals with heart conditions.
By seeking the guidance of a cardiologist, you can gain a better understanding of your condition, access specialized care, and receive the support and resources necessary to manage your heart health effectively. This professional expertise can help alleviate anxiety, build confidence in your treatment plan, and empower you to make informed decisions about your well-being.
Medication Adherence and Monitoring
Understanding Your Prescribed Medications It is crucial to have a thorough understanding of the medications prescribed for managing your heart condition. This includes knowing the purpose of each medication, its dosage, potential side effects, and any interactions with other medications or supplements.
Importance of Medication Adherence
Adhering to the prescribed medication regimen is vital for effective heart condition management. Skipping or altering doses without consulting a healthcare provider can have serious consequences and potentially worsen the condition.
Tips for Remembering to Take Your Medications
Developing strategies to help remember to take medications can improve adherence. These may include setting reminders on a smartphone or using pill organizers to keep track of daily doses.
Regular Monitoring and Follow-Up Appointments
Regular monitoring by a healthcare provider is essential to assess the effectiveness of the treatment plan, make necessary adjustments, and detect any potential complications or changes in the condition. Attending scheduled follow-up appointments is crucial for optimal heart condition management.
Building a Support Network
Engaging with Family and Friends for Support
Having a strong support network can significantly impact an individual’s ability to cope with a heart condition. Family and friends can provide emotional support, practical assistance, and encouragement throughout the journey.
Joining Support Groups and Communities
Connecting with others who are going through similar experiences can be incredibly beneficial. Support groups and online communities provide a space for sharing experiences, exchanging information, and offering mutual understanding and encouragement.
Utilizing Professional Support Services
In addition to medical care, various professional support services can aid in managing a heart condition. These may include counseling, nutritional guidance, physical therapy, and home healthcare services, depending on individual needs.
Practical Tips for Daily Living
Managing Daily Activities with a Heart Condition
Adjusting to daily life with a heart condition may require some modifications. It is essential to pace activities, prioritize rest, and seek assistance when needed. Developing strategies for energy conservation and minimizing stress can aid in managing daily tasks more effectively.
Traveling with a Heart Condition
Precautions and Tips Traveling with a heart condition requires additional planning and precautions. This may involve carrying necessary medications, obtaining travel insurance, and researching medical facilities at the destination. It is also advisable to discuss travel plans with a healthcare provider to ensure appropriate preparations.
Handling Work and Social Activities
Maintaining a balanced lifestyle, including work and social activities, is important for overall well-being. However, it may be necessary to make adjustments or accommodations based on individual limitations and recommendations from healthcare providers.
Monitoring Your Symptoms and Knowing When to Seek Help
Understanding Your Body’s Signals
Becoming attentive to your body’s signals is crucial for effective heart condition management. Being aware of changes in heart failure symptoms, such as increased fatigue, shortness of breath, or chest discomfort, can help identify potential issues early.
Knowing When to Contact Your Healthcare Provider
It is essential to know when to seek medical attention, especially if symptoms worsen or new concerning symptoms arise. Establishing clear communication channels with healthcare providers can ensure timely intervention and prevent complications.
Emergency Preparedness
What to Do in a Heart-related Emergency In the event of a heart-related emergency, such as severe chest pain or shortness of breath, it is vital to act quickly and seek immediate medical attention. Having an emergency action plan and ensuring loved ones are aware of it can help ensure prompt and appropriate response.
Using healthcare resources and systems to understand
Understanding Health Insurance Coverage Navigating the complexities of health insurance coverage can be challenging. It is essential to understand the specifics of your insurance plan, including covered services, deductibles, and out-of-pocket expenses related to heart condition management.
Planning for the Future
Long-Term Care Planning For individuals with more severe or progressive heart conditions, it may be necessary to consider long-term care planning. This can involve exploring options such as in-home care, assisted living facilities, or skilled nursing facilities, depending on individual needs and preferences.
Advanced Directives and End-of-Life Care Discussions While it may be a difficult topic, having open and honest conversations about advanced directives and end-of-life care preferences is important. This can help ensure that an individual’s wishes are respected and that loved ones are prepared to make informed decisions if necessary.
Importance of Regular Health Check-ups and Screenings Maintaining regular health check-ups and screenings is crucial for monitoring the progression of a heart condition and detecting any potential complications or additional health concerns. Early detection and intervention can significantly improve outcomes and quality of life.
Conclusion
Living well with a heart condition involves understanding your specific condition, managing physical symptoms through lifestyle changes and medication adherence, seeking emotional support, building a strong support network, and being an active participant in your care.
While a heart condition diagnosis can be daunting, it is possible to live a fulfilling life by making necessary adjustments and following the guidance of healthcare professionals. With the right knowledge, support, and determination, individuals can effectively manage their condition and maintain a good quality of life.
For comprehensive guidance and support in living well with a heart condition, individuals can consult with Dr. Ellen Mellow, one of the best heart specialist doctors in NYC, a highly experienced cardiologist who specializes in post-diagnosis management and promoting a heart-healthy lifestyle.